Healthy Paws Blog
Animal care advice for you and your pet
Learn about how to create a healthy lifestyle for your pet, the latest training methods, new treatments, and what’s new in our full-service vet surgeries in Arlington.
Explore the Healthy Paws Blog
Tags
- #CACAwesome
- Allergies
- Annual Care & Vaccinations
- Canine/Dog
- DVM Blog Post
- Exercise & Enrichment
- FAS/PVPs
- Feline/Cat
- First Aid
- Lab Work
- Medical/Sick Care
- Medications
- Microchip
- Nail Trims
- Nutrition & GI Health
- Pet Insurance
- Pet Sitters/Boarding
- Preventative Care
- Sedation & Surgery
- Socialization
- Tips & Tricks
- Training
DVM Blog Post - Coughing Cats
Just imagine, hanging with your perfect feline friend, when suddenly a weird nose that has never been heard comes out of them. Was it a hairball? How about a sneeze? An object stuck in their throat? How about a cough!
DVM Blog Post - Feline Diabetes Management
Diabetes mellitus is a familiar term to most people as it afflicts many humans. It can also be an endocrine disorder that affects dogs and cats. It is caused by a deficiency of insulin, which interrupts the normal metabolism of blood glucose (aka sugar).
DVM Blog Post - CAC in the Community
Clarendon Animal Care is exceptionally fortunate to be located in such a pet-friendly and focused community and to have such outstanding animal shelter and rescue organizations as partners - it truly makes our lives easier and even more rewarding on a regular basis!
Feline Hyperthyroidism
Hyperthyroidism is a relatively common condition that can affect middle age to older cats. It typically occurs due to overproduction of thyroid hormone.
Dr. Ungerer’s Letter to Clients
It is with mixed emotions I share with you that I will be taking on a new role in 2024, which will have me stepping back from clinical practice.
Itchy Beginnings
A new season sometimes brings a new (or recurrent) arrival of a head shake or a persistent scratch. These can be so frustrating to deal with!
Keeping the Pancreas Peppy During the Holiday Season
The holidays are once again right around the corner, which means it will soon be time for a lot of gatherings filled with food, fun, and pets if they’re excited to meet new people!
Cytology vs. Histopathology
Dogs and cats grow new lumps or bumps pretty commonly – what are we supposed to do about them? It’s absolutely reasonable to ask your veterinarian to take a peek and make recommendations.
Fleas Love Fall
We’ve discussed fleas before, but it’s a topic that never gets old and as fall tends to be when we see a spike in fleas it’s a good time to revisit.
Feeding the Felines
Obesity is one of the number one health issues we see in our feline patients, so we wanted to share a few resources, tips, and tricks.
Hypertension (aka High Blood Pressure)
Science has long shown that pet ownership can reduce our stress, boost our moods, and even lower our blood pressure. However, hypertension is a two-way street - how can we in turn help manage our own pet’s blood pressure, and why is this important?
The Advent of Veterinary Urgent Care Hospitals
One of the newest trends in the veterinary field has been that of urgent care services and stand-alone facilities. While general practitioner veterinarians are typically well-equipped to handle the full range of veterinary care - the pandemic pet boom has forced a change in this workflow.
Heartworm Disease 101
Heartworm disease is caused by a nematode parasite Dirofilaria immitis. This parasite is transmitted by mosquitoes, and makes its home in the pulmonary artery (blood vessel going from the heart to the lungs) and the right atrium (chamber of the heart).
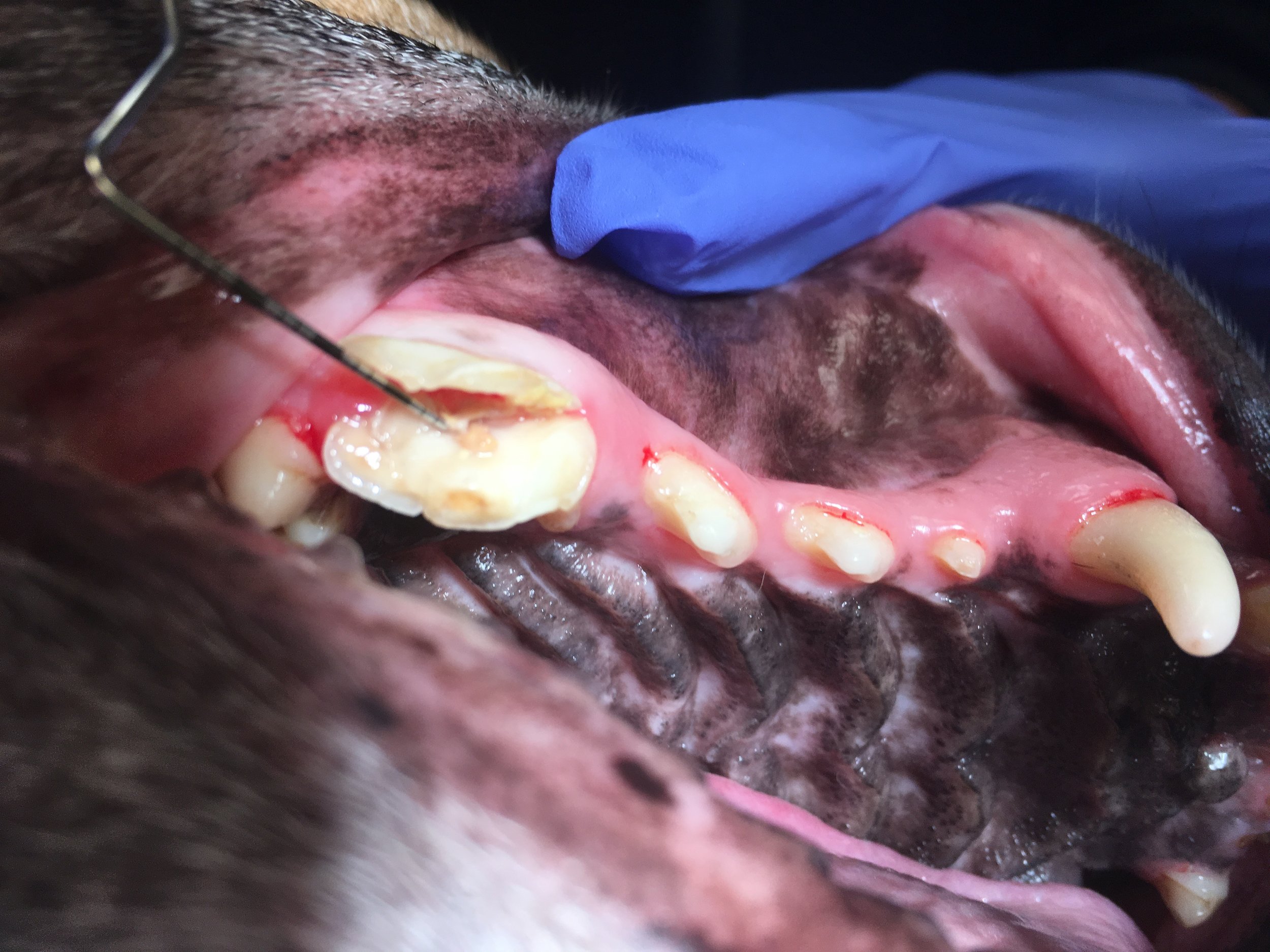
Baby Teeth Problems: Why does my dog require a surgical extraction if baby teeth are meant to fall out?
Baby Teeth Problems: Why does my dog require a surgical extraction if baby teeth are meant to fall out?
Routine Fecal Testing
Believe it or not, there’s a week coming up in April honoring “National Scoop the Poop Week,” from April 23-29, 2023. While this may seem a bit humorous, unscooped dog waste is no laughing matter.
Veterinary-Client-Patient Relationship (VCPR)
Just as in the human medical field, a veterinarian must have a valid Veterinary-Client-Patient Relationship (VCPR) established in order to provide medical recommendations and prescribe medications for a patient.
Common Household Toxins
There are many resources available covering potential household toxins, but we wanted to elaborate on several of these potentially lesser-known items of concern.
August 2022 Newsletter
With summer travels upon us, many of us are left wondering how best to care for our pets while we’re out of town; whether to bring them along, leave them at home, or to board them - the decision can be hard to make!
Cats Need Exercise Too!
Did you know that household cats, especially those who live exclusively indoors, have little to do and can easily become bored? This can lead to behavioral issues, excessive weight gain, and eventual health consequences. Although it may be tempting to allow your cat outdoors, there are many safety and health concerns that pose a much higher risk than keeping your cat indoors.
July 2022 Newsletter
With summer travels upon us, many of us are left wondering how best to care for our pets while we’re out of town; whether to bring them along, leave them at home, or to board them - the decision can be hard to make!
Cushing’s Syndrome
Cushing’s Syndrome (also known as hyperadrenocorticism) is a condition that primarily affects older dogs. It is caused by an overproduction of hormones by the adrenal glands. The most common cause is a small tumor on the pituitary gland that sends signals to the adrenal glands to overproduce hormones.
June 2022 Newsletter
Summer vacation is upon us and for many that means upcoming travel! If you are choosing to bring your pet on your trip, we recommend some pre-trip preparation.
What is Feline Stomatitis?
Feline stomatitis is a painful inflammatory disease of the mouth that we see in cats infrequently. When severe, cats can lose weight, have bad breath, drool, drop food, eat less or stop eating, hiss or vocalize at their meals, and stop grooming.
May 2022 Newsletter
May is National “Chip Your Pet Month”! While most of us like to assume that our pets will always be safe and at home, there are chances that your pet may end up lost, stolen, or on a “field trip” around your neighborhood at some time or another.
Pet Insurance
One of the best things a pet owner can do for their pet and themselves is get pet insurance! We consider pet insurance to be an important investment in the lifetime medical care of your pet and recommend coverage for all our patients.
April 2022 Newsletter
Spring has sprung and so have allergies! As we enter the warmer months, you may notice your pet sniffling, sneezing, and even licking more!
April is National Pet First Aid Awareness Month
April is National Pet First Aid Awareness Month. The first step in knowing if there is a problem is knowing what is normal for your pet.
March 2022 Newsletter
Kicking off the month of March may mean four leaf clovers and green beer to most of us, but it’s also Pet Poison Prevention Awareness Month!
What Is That?! - Peri-renal Fat Pads
Have you ever experienced this embarrassing situation? You schedule an appointment with your veterinarian because as your dog has gotten older, she has developed two symmetrical lumps over her hips…
What Is That?! - Anal Sacs
So many pet owners have been there…You’re sitting in your living room watching TV while snuggling with your best bud, when all the sudden you hear a startling noise. You both jump with fright, but soon realize it was just…
The Chew on Chew Toys
Chances are that, in addition to chasing squirrels and keeping watch over the Amazon package delivery man, one of your dog’s favorite pastimes is chewing. Bones, rawhides, sticks…
Can I catch that from my pet? - No!
Can I catch that from my pet? This is a common question we hear as veterinarians, and as such have made this a recurring topic. This week we debunk some myths…
Can I catch that from my pet? - MRSA
Can I catch that from my pet? This is a common question we hear as veterinarians, and as such have made this a recurring topic. This week we cover antimicrobial resistance…
What Is That?! - Third Eyelid
A few weeks ago we started a new series in our column aptly named, “What Is That?!”. Our goal is to shed light on some of the anatomical oddities that veterinarians are frequently asked about…
Pet New Year's Resolutions
It’s January and the time for new year resolutions. While you may a few on your own list, have you thought about resolutions…
What Is That?! - Incisive Papilla
One of the most important topics studied in vet school is anatomy - as veterinarians, we need to know what is normal and what isn’t. Most pet owners…
Can I catch that from my pet? - Toxoplasmosis
Can I catch that from my pet? This is a common question we hear as veterinarians, and as such have made this a recurring topic. This week we cover Toxoplasmosis… for a few reasons…
These are a few of my favorite things...
It’s that time of year again! Time to embrace the season and ponder on the best gift…
Can I catch that from my pet?
Can I catch that from my pet? This is a common question we hear as veterinarians. So, we’re going to make…
Halloween - The Recap
Well - we couldn’t have asked for better weather last night for a little trick or treating! And we couldn’t have asked for better entries…
Obesity in Our Pets: An Ounce of Prevention is Worth a Pound of Cure
A study conducted by the Association for Pet Obesity and Prevention found that 56% of dogs and 60% of cats in the United States were classified as overweight…
Cannabidiol - is it really the greatest thing since sliced bread?
We are frequently asked about CBD, or cannabidiol, particularly in the form of CBD oil, and its various benefits. As this is still…
Safe Disposal of Medicines and Preventing Environmental Contamination
Although still undergoing much research, it is clear that chemical pollutants are impacting the environment, animal health, and…
Summers End
With the unofficial end of summer this week, it’s time to look at what changes and challenges…
Dog Park 101
The dog park a super fun place to bring your puppy for exercise and socialization with other dogs, but there are some things…
Pet Nutrition and Heart Disease - Connection or Coincidence?
Earlier this year, Peanut, a 4-year-old male Beagle/Lab mix was diagnosed with a life-threatening…
Leptospirosis
It’s finally summer time, and nothing means summer quite like playing in puddles, creeks, and rivers. But keep in mind… [READ MORE]
Preparing for the 4th of July
A good rule of thumb is that your dogs and cats likely don’t want to watch the fireworks with you and should not
How the Opioid Epidemic is Affecting Veterinary Medicine...
The opioid epidemic has been in the new quite a bit recently, and for good reason. While opioid, and other prescription drug abuse, is of significant concern… READ MORE
Blue the Elder Dog
Sometimes being a Revisionary Gerontologist can get me down. There are a lot of things that need to change in how we see people as they grow older… READ MORE
It's National Pet Week!
The American Veterinary Medical Association has declared May 6th-12th National Pet Week… READ MORE
Summer Tips
Though Summer is technically almost 2 months away, with the weather we’ve had the last few days it already feels… READ MORE
Did You Know...?
This week we thought we’d present a few fun facts about the amazing furry creatures many of us share our lives with... READ MORE
Understanding Your Pet's Labwork Results - Part II: Basic Chemistry Panel
A couple of weeks ago we looked at the significance of the complete blood cell count. This week, we’ll be looking at the serum chemistry profile, which has... READ MORE
Understanding Your Pet's Labwork Results - Part I: The CBC
Many pets have had bloodwork run at some point in their life - perhaps prior to routine surgery such as neutering, or possibly... READ MORE
Boy Dog Bumps - The Mysterious Bulbus Glandis
Have ever experienced this scenario? You have a wonderful new male puppy and one day he rolls over for a belly rub and you notice these two round swollen bumps... READ MORE
February is Pet Dental Health Month!
Ever wondered what that smell was permeating from your pet’s mouth!? Bad breath is a very common complaint among... READ MORE
Puppy Love and Kitty Snuggles...Interesting Facts about the Human-Animal Bond
February is the month of LOVE, and who better to shower love on than your pets! Human-Animal relationships...
Choosing the Right Collar or Harness
Leash pulling is a common and frustrating dog behavior, but walking calmly on a leash is not a natural instinct for dogs and learning...
The Dreaded Nail Trim
Taking your pet in for a nail trim - it sounds so simple, and for many dogs and cats it is. But, for others, it is truly a terrifying...
New Years Resolutions - Pet Edition
2017 is almost over and we’ll be in a new year next week. What are your resolutions?...
Fur-baby, it's cold out there!
Winter is finally here and we cannot stress enough the importance of keeping pets in a warm, protected environment this time of year. So, for this week’s post, we’re reminding...
Online Pet Pharmacies
Online, 3rd party, pet pharmacies such as 1-800-Petmeds, Allivet, and many others, have become very popular over the recent years, and with good reason. They often are able to offer lower prices...
Antibiotic Use in Pets
November 13 - 19 has been declared World Antibiotic Week. While at first glance it might be easy to roll your eyes at this...